Glucotrack
Implantable Glucose Monitor
Hardware and firmware development for a first-in-human implantable glucose monitor with 3-year battery life.

Continuous glucose monitors available today measure glucose from interstitial fluid, introducing a lag that limits accuracy for people on intensive insulin therapy. Glucotrack is developing a fundamentally different approach: a fully implantable CBGM that measures glucose directly from the bloodstream, with a 3-year sensor lifespan and no external wearable component. Achieving this required solving a tightly coupled set of engineering challenges, from designing electronics compact enough to be implanted, to developing firmware capable of reliable BLE data transmission and continuous sensing, all within the strict energy constraints of a long-term implantable device.
Glucotrack needed hardware and firmware for a fully implantable glucose monitor designed to survive years inside the human body.
What We Built
Focus developed the hardware and firmware for an implantable continuous blood glucose monitor (CBGM) through its first-in-human (FIH) product phase. The resulting device successfully completed verification testing and has been deployed in multiple clinical trial studies. Focus continues to advance both the hardware and firmware for subsequent product phases leading to commercialization. The primary design challenges centered on achieving an extremely compact form factor, while balancing continuous glucose monitoring with stringent low power constraints. This required developing ultra-low-power hardware and firmware capable of reliably acquiring glucose measurements and transmitting data via Bluetooth Low Energy (BLE) to a companion mobile application, all within the battery limitations of an extremely low power implantable medical device.

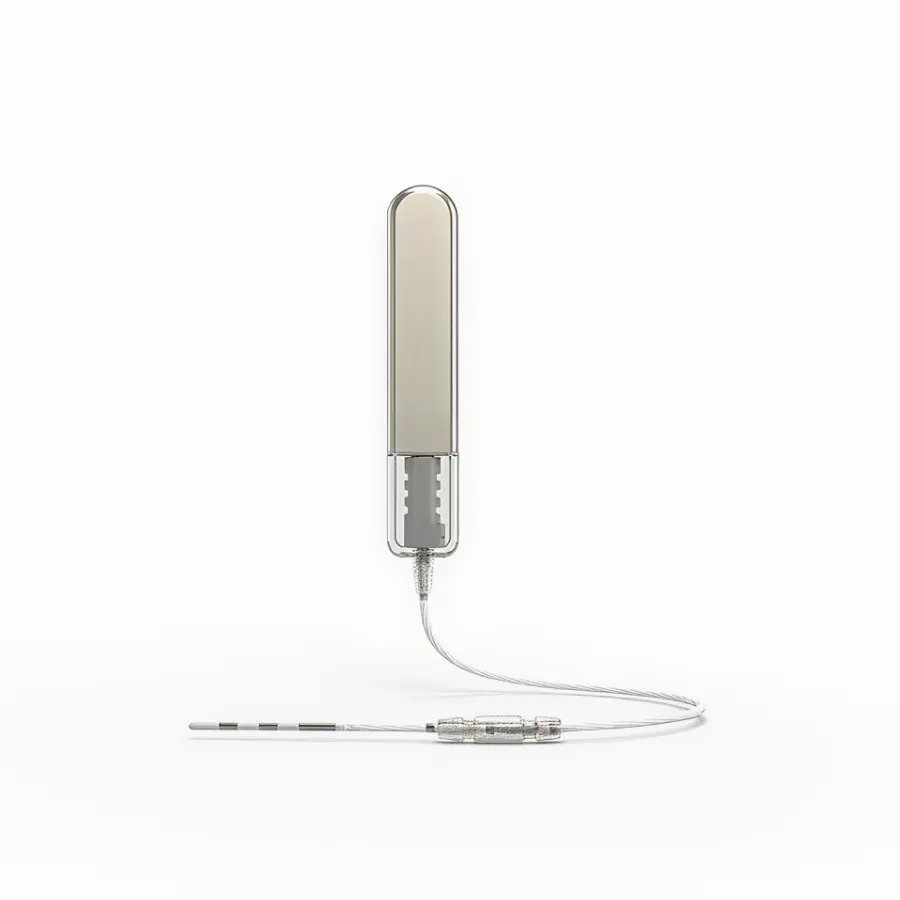

Impact
The developed CBGM implantable device has been successfully used in human clinical trials, demonstrating potential to set new standards in diabetes care by improving user experience and convenience. Preliminary feedback has been overwhelmingly positive, reflecting strong market demand and user approval for the technology.
3-Year Battery Life Target
Ultra-low-power hardware and firmware optimization enabled a device designed for over three years of continuous operation, eliminating the frequent replacement burden that limits every CGM solution currently on the market.
7.7% MARD in First-In-Human Trial
Clinical results showed a 7.7% mean absolute relative difference across 122 matched pairs, with 92% of readings in the clinically acceptable green zone of the Diabetes Technology Society Error Grid.
99% Data Capture Rate
Near-complete data availability across the full study period validated the firmware's reliability and power management under real implant conditions, confirming that BLE performance held consistently inside the human body.

Achieving three-plus years of continuous, accurate blood glucose monitoring in a fully implantable device required solving some of the hardest tradeoffs in low-power electronics and embedded firmware design.

